What is voluntary patient safety event reporting?
Voluntary Patient Safety Event Reporting is a method of collecting details and information about an incident, near miss or unsafe condition in hospitals and other care settings through an electronic or paper-based form submitted by frontline staff.

As research published in 2020 by the Journal of Patient Safety acknowledged, “A natural, human tendency when errors have occurred is to ignore or minimize the error. It takes a lot of work to build an environment that supports the opposite reaction: open and honest reporting of errors so they can be evaluated to contribute to organizational learning.”
It’s counterintuitive but inescapable: To achieve the highest levels of reliability, High Reliability Organizations must defy human nature by eagerly embracing the evidence of failure. This article will suggest six strategies, and even more specific techniques, for creating a culture that encourages — and even incentivizes — team members at all levels to report incidents, near misses and unsafe conditions.
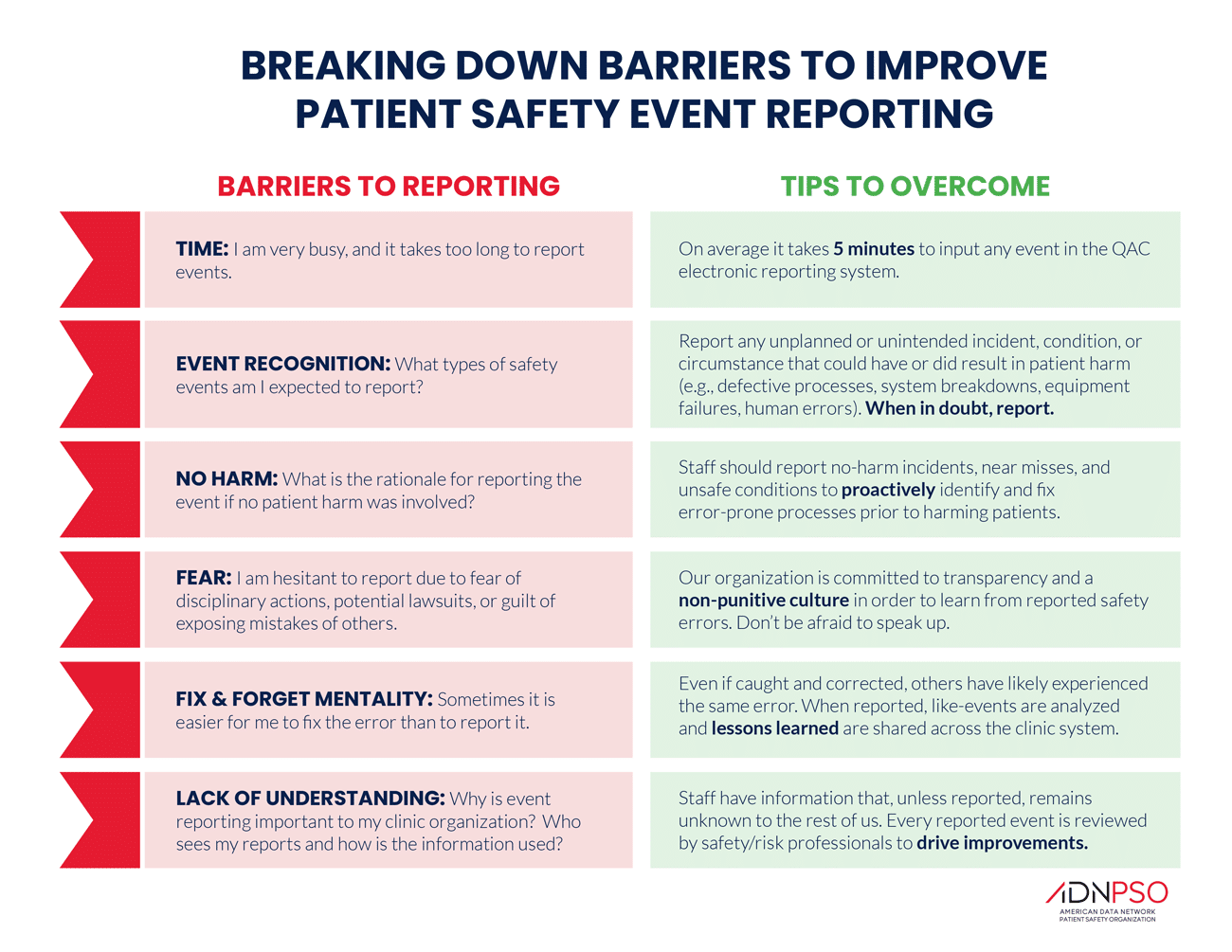
Encouraging and incentivizing reporting requires first understanding the reasons that team members may fail to do so. As the graphic below illustrates:
- Team members must understand the big picture of preventing future patient safety events by analyzing and sharing past errors. Preoccupation with failure is a mindset that must be fostered at every level. Reporting of safety events and concerns must be recognized as a critical component of patient care.
- Team members must be assured that reporting will not create problems — for themselves, their coworkers or the facility. Fear of immediate personal repercussions is a disincentive to future patient safety. If you want to trust your staff to report safety concerns and events, your staff must trust that they will not regret reporting. Snitches prevent stitches!

What strategies and tactics work?
- Regular education and reinforcement
Awareness of patient safety as a science that must be taught and reinforced has been growing, but your hospital or clinic is an amalgam of patient care providers whose immersion in the mindset and culture of patient safety cannot be assumed. Your facility’s safety culture and processes for reporting issues must be central to the onboarding and orientation process.
As writer Susan Trossman described in a 2017 article in The American Nurse, cultural expectations like engaging in daily safety huddles and working collaboratively must be communicated to new hires and then reinforced in continuing training and routine communication. (Her article also describes an added benefit of intensive orientation, at least with nurses: higher rates of employee retention.)
Safety champions — engaged team members with specialized training — are a tried and true method of reinforcing your desired culture of safety, including normalizing routine reporting of events. Appointing champions per department or location is a great way to ensure the focus on reporting gets regularly communicated on the front lines.
- Evidence of effectiveness
Proving to your staff that their reports of errors and near misses don’t disappear into the ether creates a virtuous feedback loop: Reporting results in improvements, which results in more reporting. An analysis of data from more than 200,000 individuals in almost 1,000 hospitals concluded that prioritizing feedback to reporters is one of the most efficient ways to increase the likelihood that a patient safety event will be voluntarily reported. And this was especially true with the most serious patient safety events. (While you are at it, consider using language such as “safety report” rather than “incident report.”)
- Convenient and natural reporting opportunities
You may be familiar with “nudge theory,” the idea that desired behaviors can be fostered by making them more convenient. (This explains the candy bars in the checkout aisles of grocery stores — and Best Buy.) The desired outcome of voluntary reporting of patient safety events can also be nudged by creating convenient, natural reporting opportunities.
One common and effective strategy is the daily huddle, in which patient safety is the central agenda item for all team members. Periodic observation to make sure daily huddles are being used to encourage event and near-miss reporting is a good management technique. Consider adding the daily question: “How is the next patient going to be harmed?”
Anything that requires a lot of time and effort will always take a backseat to the urgency of patient care, so convenient reporting can also be encouraged with user-friendly reporting technology. This free Patient Safety Event Reporting Gap Analysis template can help you conduct a thorough evaluation of how well or poorly your existing tool or process accomplishes the necessary objectives of an event reporting system.
- Management encouragement
Hearing the gospel of voluntary reporting from evangelists at the top of your organization is key to creating and sustaining a culture of patient safety. These messages from leadership are an opportunity to dispel the fear of retribution from reporting events and instead help promote a just culture at your facility. ADN’s Increase Event Reporting Toolkit can help with templates for emails from senior leaders. Hanging posters reminding frontline staffers of the types of events they should report can keep the responsibility for reporting top of mind. (The toolkit also contains a poster template.)
Every communication channel in your organization is an opportunity for reinforcing the message: staff meetings, intranet, newsletters, etc. But it won’t get done unless someone is specifically tasked with adding safety to the to-do list. Staff meeting agendas and newsletters often feature standing items that carry over from one to the next; voluntary reporting should be one of those standing items.
- Recognition and reward programs
Behavior rewarded is behavior repeated. Recognition of voluntary reporting through “good-catch campaigns” can take the form of certificates or plaques and even that most prized reward: a paid day off for the staff member who reports the best good catch each quarter.
If your state has a patient safety recognition program, be sure your good catches are entered. Whether your staff member is ultimately recognized statewide or not, knowing that their focus on safety has not been forgotten reinforces the original recognition.

- Intensive Reporting Days
It may seem counterintuitive in a culture that encourages reporting of incidents and near misses year-around, but designating intensive reporting days results in more reporting. Research published by the Journal of Patient Safety found that it works at all levels of an organization, especially when reporting can be done conveniently and anonymously.
Clinicians, staff members and patients in 10 family medicine clinics were encouraged to make routine reports during a 10-week study, but they were asked to report every error on five specific days. Their anonymous reports could come through a website, paper forms or a voice-activated phone system. During the 70-day study period, more than a third of the reports came on the five days that were designated for intensive reporting.
ADN’s Increase Event Reporting Toolkit includes an Intensive Reporting Day checklist and support materials to help your organization take advantage of this proven technique for improving voluntary reporting.

Then what?
As you implement new strategies and techniques to improve voluntary event reporting, you can track overall improvement and even compare your facility to other hospitals using ADN’s Patient Safety Event Reporting Rate Calculator. The calculator shows how far above or below average your event reporting rate is as well as suggested reporting rate improvement goals and more recommended strategies, tactics and tools based on your facility’s performance.